Aortic Valve and Aorta Replacement
Case Study 1:
Aortic Valve Replacement with Ascending Aorta Replacement
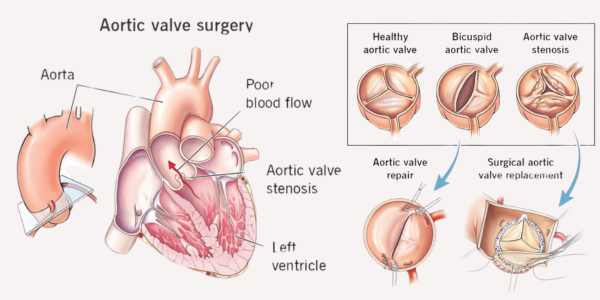
Medical illustration showing aortic valve stenosis, its effect on blood flow from the left ventricle to the aorta, comparison of healthy and diseased aortic valves, and surgical options including aortic valve repair and valve replacement.
A successful surgical management of a complex cardiac condition involving severe aortic valve disease with ascending aortic dilation. Through timely diagnosis, expert surgical care, and structured postoperative management, the patient achieved an excellent recovery and returned to a normal, symptom-free life.
Patient’s Background and Health Concerns
A 55-year-old male patient lived with ongoing physical discomfort for several years. Starting in 2018, the symptoms slowly worsened over time and affected daily activity. The main health concerns reported by the patient included the following symptoms:
- Generalized weakness
- Early fatigue
- Shortness of breath on mild exertion
These symptoms continued for a few years and did not improve on their own. The repeated weakness and breathlessness limited normal movement and effort. This gradual progression pointed toward a heart condition that required further medical evaluation.
Diagnosis and Medical Assessment
A detailed cardiac evaluation was carried out to identify the cause and severity of the patient’s condition. Multiple diagnostic tests were used to assess heart function, valve status, and aortic anatomy. The findings helped confirm the extent of valve disease and aortic involvement. The following investigations were used for medical assessment:
- Electrocardiogram (ECG)
- Chest X-ray (CXR)
- Transthoracic Echocardiography (Color Doppler)
- CT Angiogram of the heart and great vessels
- CT scan of the chest with contrast
- Coronary Angiogram
- Routine blood tests
The combined results showed severe aortic stenosis with ascending aortic dilation. These findings explained the patient’s long-standing symptoms and supported the need for surgical treatment to prevent further clinical deterioration.
Treatment Plan and Surgical Procedure
Surgical treatment was advised after reviewing all diagnostic findings. The patient was admitted on 21 October 2025 for planned cardiac surgery. The operation was scheduled based on disease severity, symptom duration, and test results showing advanced valve and aortic involvement.
The operation was performed on 23 October 2025 by Dr. Mohammad Moniruzzaman, MBBS, MS (Cardiovascular & Thoracic Surgery).
The procedure took place at Ship International Hospital under standard cardiac surgical protocols and involved coordinated support from anesthesia and critical care teams.
Open-heart surgery was performed using cardiopulmonary bypass. A 25 mm ON-X mechanical valve was used to replace the diseased aortic valve. The dilated ascending aorta was replaced with a 26 mm PTFE tube graft during the same procedure.
The surgical steps were completed in a controlled manner. The patient was successfully weaned off cardiopulmonary bypass without difficulty. No intraoperative complications were noted during valve replacement or aortic reconstruction.
After surgery, the patient was transferred to the Cardiac Intensive Care Unit for close monitoring. Postoperative care focused on hemodynamic stability, pain control, and early recovery support under continuous medical supervision.
Outcome and Patient’s Current Health Condition
The postoperative period remained smooth and uneventful from the early recovery phase through discharge. Clinical monitoring showed stable progress without complications.
Recovery milestones were achieved on time, allowing planned step-down care and safe discharge within the expected hospital stay. The following recovery milestones were observed during the postoperative period:
- Extubation on the following morning
- Chest drain removal on the second postoperative day
- Temporary pacing wire removal on the fifth postoperative day
Postoperative care focused on gradual recovery and daily assessment. Each recovery step was completed without delay or adverse events. The patient remained clinically stable throughout the hospital stay and was discharged on the tenth postoperative day, dated 3 November 2025.
After discharge, complete relief from previous symptoms was noted. Weakness and shortness of breath resolved fully. Physical activity tolerance improved, and the patient resumed normal daily activities while remaining under routine medical supervision.
Regular follow-up remains part of ongoing care. The next scheduled visit is on 20 March 2026. The visit will include clinical assessment and routine investigations to monitor recovery and long-term surgical outcomes.